Aging often brings with it various health complications, with older women especially facing unique challenges. Notably, endocrine problems represent one such difficulty.
1. Endocrine Problem Osteoporosis: The Silent Disease
Understanding Osteoporosis in Older Women
Osteoporosis, an endocrine disorder, quietly affects millions of older women around the globe. This chronic condition stealthily diminishes bone strength and integrity over time.
Recognizing the Symptoms of Osteoporosis
Women often have no visible symptoms in the early stages of osteoporosis. As the disease progresses, though, they may start to notice a few changes. Height loss, an unexpected stoop, or sudden back pain can all indicate osteoporosis. Fractures can occur even with minor trauma, especially in the hip, spine, and wrist.

Risk Factors Specific to Women
Certain risk factors increase the likelihood of developing osteoporosis. For women, these risk factors can involve endocrine factors, lifestyle choices, and certain medical conditions. Menopause is an important endocrine event that can accelerate bone loss due to a decrease in protective estrogen levels. Prolonged inactivity, low calcium intake, and excessive alcohol consumption also contribute to the development of osteoporosis.
The Role of Endocrine System in Osteoporosis
The endocrine system, with hormones like estrogen and parathyroid hormone, play a critical role in maintaining bone health. Estrogen loss during menopause can negatively affect bone density. The parathyroid hormone regulates calcium levels, and an imbalance can cause calcium to be drawn from the bones, thus leading to osteoporosis.
Diagnosing Osteoporosis in Older Women
Healthcare providers typically diagnose osteoporosis through bone density tests. These tests measure the amount of calcium and other bone minerals packed into a segment of bone. The lower the bone mineral density, the greater the risk of fractures.
Treatment Options for Osteoporosis
The treatment for osteoporosis usually aims to slow or stop bone loss, prevent fractures, and reduce pain. Doctors often recommend calcium and vitamin D supplements to ensure adequate bone nutrition. Hormone-related therapy, particularly estrogen therapy, can be beneficial for post-menopausal women.
Physical exercise, particularly weight-bearing and muscle-strengthening exercises, can help build and maintain bone density. Certain medications, like bisphosphonates, can inhibit bone breakdown and preserve bone mass.
Living with Osteoporosis
Living with osteoporosis involves taking steps to prevent falls that might cause fractures. Older women should make their living spaces safer, wear low-heeled shoes with non-slip soles, and ensure adequate lighting in their homes.
Despite being an endocrine and metabolic disorder, osteoporosis is not a definitive life sentence. With early diagnosis, effective treatment, and lifestyle modifications, older women can manage osteoporosis and lead active, fulfilling lives.
2.Endocrine Problem Menopausal Symptoms: A Marked Transition
Understanding Menopause in Older Women
Menopause signifies the end of a woman’s reproductive years, typically happening between the ages of 45 and 55. As the ovaries cease estrogen production, the endocrine system undergoes a significant transformation. This shift triggers various physical and psychological changes, most pronounced in older women.
Identifying the Symptoms of Menopause

Emotional and Psychological Changes
Endocrine shifts in menopause can also affect mental well-being. Some women may undergo mood swings, depression, and anxiety. Difficulty in concentration and memory lapses are not uncommon, often referred to as “brain fog”. Recognizing these emotional symptoms is as crucial as understanding the physical ones.
Bone Health and Menopause
The decline in estrogen production affects bone density, leading to a higher risk of osteoporosis. This condition causes bones to become weak and fragile, potentially leading to fractures. Regular weight-bearing exercises and maintaining a balanced diet rich in calcium and vitamin D can help protect bone health.
Cardiovascular Risks
Post-menopause, there’s an increased risk of developing cardiovascular conditions due to the changes in the endocrine system. As estrogen has a protective effect on the heart, its decrease can lead to higher cholesterol levels, increased blood pressure, and a higher risk of heart disease.
Treating Menopausal Symptoms
Management of menopausal symptoms varies based on their severity and impact on quality of life. Hormone replacement therapy (HRT) can alleviate symptoms by supplementing the body’s declining estrogen levels.
Despite the benefits of HRT, it’s important to remember that it isn’t suitable for everyone and the potential risks associated with it demand thoughtful consideration.
As an alternative, non-hormonal medications can step in to help manage specific symptoms. In the same vein, antidepressants have the potential to mitigate hot flashes and bolster mental well-being. Moreover, when the situation calls for it, medications for osteoporosis and heart disease can be put into use.
Simultaneously, lifestyle changes play a pivotal role in managing menopausal symptoms. This includes engaging in regular exercise, sticking to a balanced diet, maintaining proper hydration, and placing importance on sleep. These activities collectively contribute to enhancing overall health and well-being during menopause.
Nonetheless, it is crucial to understand that menopause is a natural part of aging, causing noticeable shifts in older women due to the ever-changing endocrine landscape. Recognizing these changes and seeking appropriate treatment can significantly enhance the quality of life during this phase.
3. Thyroid Disorders due to Endocrine Problems: An Overlooked Problem
Recognizing Thyroid Disorders in Older Women
Thyroid disorders constitute a common but often overlooked endocrine issue in the geriatric population, especially among women. Age-related changes can affect the structure and function of the thyroid gland, leading to various health issues.
Symptoms of Thyroid Disorders
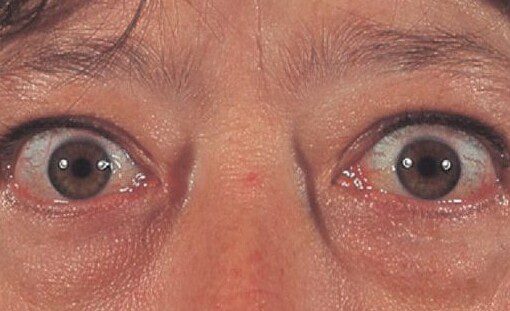
Diverse symptoms accompany thyroid disorders in older women. For hyperthyroidism, symptoms may include rapid heart rate, weight loss, increased appetite, tremors, and sweating. In contrast, hypothyroidism symptoms can manifest as fatigue, constipation, weight gain, depression, and cold intolerance. However, these symptoms often mimic signs of aging, making diagnosis challenging.

Specific Thyroid Disorders in Older Women
Among the endocrine disorders, hyperthyroidism and hypothyroidism hold a high prevalence. Hyperthyroidism results from an overactive thyroid gland that produces excessive thyroid hormone. Graves’ disease is a common cause in older women. Hypothyroidism, on the other hand, results from an underactive thyroid gland that fails to produce adequate thyroid hormone. Hashimoto’s thyroiditis often underlies this condition.
Importance of Timely Diagnosis
Timely diagnosis of these endocrine disorders is critical. Without proper intervention, they can exacerbate comorbid conditions common in older age, like heart disease or osteoporosis. They might also increase the risk of cognitive impairment or affect emotional well-being.
Diagnostic Measures
Diagnosis usually involves blood tests to evaluate levels of thyroid-stimulating hormone (TSH) and thyroid hormones (T3 and T4). Occasionally, imaging studies or a thyroid scan may supplement these tests to rule out causes such as nodules or cancer.
 Treatment of Thyroid Disorders
Treatment of Thyroid Disorders
Treatment strategies for thyroid disorders in older women involve managing the underlying cause and alleviating symptoms. Hyperthyroidism treatment options may include anti-thyroid medications, radioactive iodine therapy, or in rare cases, surgery. These methods aim to reduce the overproduction of thyroid hormones.
On the other hand, hypothyroidism requires hormone replacement therapy with levothyroxine to supplement the deficiency of thyroid hormones. The key to successful treatment lies in individualized dosing and regular monitoring to avoid overtreatment or undertreatment.
Thyroid disorders are a significant endocrine issue affecting older women. The subtle onset of symptoms and their overlap with typical aging signs necessitates heightened vigilance. Comprehensive diagnostic measures and personalized treatment plans are crucial for effective management. By increasing awareness and improving healthcare access, we can ensure optimal health for older women battling these endocrine issues.
4. Endocrine Problem Type 2 Diabetes: A Growing Concern
Understanding Type 2 Diabetes in Older Women
Type 2 Diabetes is an endocrine disorder that affects many older women. The condition originates from the body’s ineffective use of insulin, which ultimately leads to elevated blood sugar levels.
Recognizing Symptoms of Type 2 Diabetes
A variety of symptoms can suggest the onset of Type 2 Diabetes. They often develop slowly, making them difficult to notice. These symptoms include frequent urination, increased thirst, constant hunger, unexplained weight loss, fatigue, blurred vision, slow-healing sores, and frequent infections.
The Role of the Endocrine System in Type 2 Diabetes
The endocrine system plays a vital role in managing our body’s insulin levels. In Type 2 Diabetes, the body’s insulin resistance disrupts the endocrine system’s usual regulation of blood sugar levels. This disruption can lead to a range of complications if left untreated.

Potential Risks and Complications
Untreated or poorly managed Type 2 Diabetes can result in various complications. These may include heart and blood vessel disease, nerve damage (neuropathy), kidney damage, eye damage, slow wound healing, and hearing impairment. Women with Type 2 Diabetes also face an increased risk of Alzheimer’s disease.
Screening and Diagnosis of Type 2 Diabetes
For older women, regular screening for Type 2 Diabetes is crucial. Your healthcare provider will administer a blood test to measure your fasting blood sugar levels. If the results indicate a higher level than normal, they might conduct an oral glucose tolerance test or an HbA1c test to confirm the diagnosis.
Treatment Approaches for Type 2 Diabetes
Effective management of Type 2 Diabetes involves several lifestyle changes and treatments. These include maintaining a healthy diet, regular physical activity, and weight management. Medications may also be prescribed to control blood sugar levels and to handle any complications.
For older women, doctors might recommend medication adjustments in response to the body’s changing endocrine functions. Treatments may also focus on managing other age-related conditions that could exacerbate diabetes.
Coping with Type 2 Diabetes
Living with Type 2 Diabetes requires consistent management. Regular monitoring of blood sugar levels, a well-balanced diet, and an active lifestyle can help control this endocrine disorder. Support groups and counseling may also be beneficial to address any psychological stress related to managing the disease.
Remember, each woman’s experience with Type 2 Diabetes will be unique. Your doctor will tailor your treatment plan to meet your individual needs, focusing on maintaining a healthy and balanced endocrine system.
5. Weight Gain and Obesity: An Underestimated Threat
Endocrine Problems and Obesity in Older Women
Endocrine disorders can influence weight gain and obesity in older women. Conditions such as hypothyroidism, Cushing’s syndrome, and polycystic ovary syndrome (PCOS) often culminate in unanticipated weight gain. These issues are especially common among older women, emphasizing the need for effective diagnosis and treatment.
Recognizing Symptoms of Hypothyroidism
Hypothyroidism is a condition where the thyroid gland does not produce enough thyroid hormone. This deficiency can cause a slow metabolism, leading to weight gain. Older women may experience symptoms like fatigue, constipation, and cold intolerance.
Cushing’s Syndrome: An Overlooked Issue
Cushing’s syndrome, another endocrine disorder, is caused by high cortisol levels over an extended period. It frequently results in weight gain, particularly in the upper body and around the neck. Additional symptoms include muscle weakness, a rounded face, and thin skin that bruises easily.
The Impact of Polycystic Ovary Syndrome
Polycystic ovary syndrome, though typically diagnosed in younger women, can persist into later years. Its impact on the endocrine system can lead to weight gain. Symptoms of PCOS include irregular periods, excessive hair growth, and acne.
Addressing Weight Gain and Obesity
Understanding the root cause of weight gain and obesity in older women is essential. Diagnosis typically involves blood tests to check hormone levels. Radiology scans may be necessary to visualize the endocrine glands. After diagnosing the underlying endocrine disorder, an appropriate treatment plan can be developed.
Treatments for Hypothyroidism
Hypothyroidism treatment typically involves daily use of the synthetic thyroid hormone levothyroxine. This medication restores adequate hormone levels, reversing the symptoms of hypothyroidism. Consequently, it can help manage weight gain associated with the disorder.
Managing Cushing’s Syndrome and PCOS
Treatment for Cushing’s syndrome depends on the cause. If medication is the source of excessive cortisol, doctors may adjust the dosage or switch to a different drug. In some cases, surgery might be necessary. Losing weight can also help manage the symptoms of Cushing’s syndrome.
For PCOS, lifestyle changes are often the first line of treatment. These include eating a healthy diet and regular exercise to promote weight loss. Certain medications might also be prescribed to manage symptoms.
Endocrine disorders are a common source of weight gain and obesity in older women. By identifying these conditions early, doctors can prescribe appropriate treatments to manage weight gain and improve overall health. Education and awareness are key to understanding the role of the endocrine system in maintaining a healthy weight.

Taking Control: Health Management Strategies
Dealing with these endocrine disorders requires a combination of lifestyle changes, medical interventions, and routine check-ups. Adequate calcium and vitamin D intake can help reduce the risk of osteoporosis. Regular exercise aids in maintaining a healthy weight and improving insulin sensitivity. Physicians can provide hormone replacement therapy for managing menopausal symptoms. Regular blood tests can ensure early detection of thyroid disorders and diabetes.
With knowledge and the right strategies, older women can navigate these endocrine issues and continue to lead fulfilling lives.