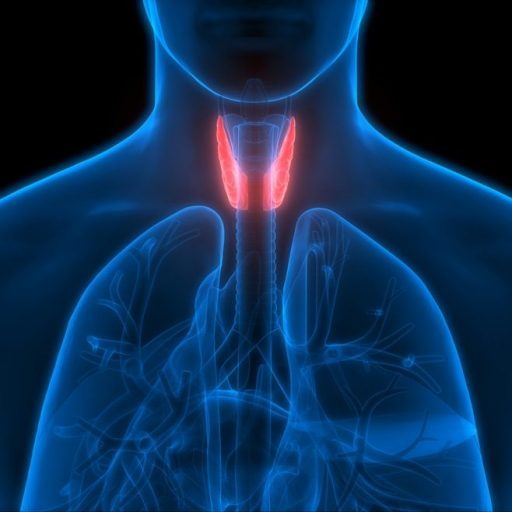
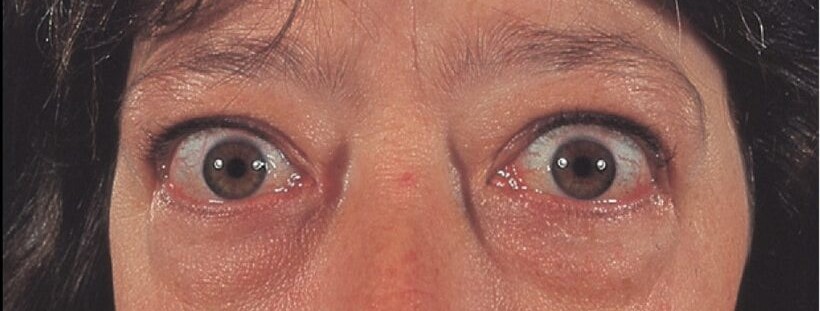
In 1835 Robert Graves, a British physician, described signs of thyroid disease including exophthalmos (forward protrusion of the eyes), and his name has become an eponym for an eye condition associated with thyroid dysfunction. Although most frequently associated with hyperthyroidism, this eye condition (Graves’ ophthalmopathy) can occur in patients with no laboratory evidence of thyroid dysfunction.
Background and History of Graves’ Disease
A major feature of Graves’ disease is the presence of changing eye signs and symptoms. Remissions and exacerbations are signs of varying degrees of orbital inflammation and are characteristic features of Graves’ ophthalmopathy.
Eye symptoms often coincide with thyroid disease. However, they can also either precede or follow its detection. This detection is usually made from blood hormone level abnormalities.
Interestingly, the emergence and progression of Grave’s eye disease don’t typically mirror that of systemic thyroid disease. Generally, most thyroid patients aren’t afflicted with eye disease. And if they are, it’s typically mild. Regrettably, there’s no way to foresee who it will impact.
Studies have indicated that this eye disease is more prevalent in women who smoke. Furthermore, the severity of the condition tends to increase in these individuals. Although the eye and thyroid conditions are facets of the same disease, treating the thyroid gland successfully doesn’t assure eye improvement.
Sadly, no thyroid treatment method reduces the likelihood of eye involvement. Once inflamed, the eye disease might stay active for several months. It can even persist for up to three years. Afterwards, there might be partial or complete improvement.
After Grave’s ophthalmopathy has become inactive for six months, recurrence of eye disease is infrequent and may coincide with poor control of thyroid hormone levels.
Pathophysiology Graves’ Disease
The pathophysiology of the eye findings of Graves’ disease remains obscure. Inflammation and edema of the orbital tissues, especially the extraocular muscles, result in significantly increased tissue volume within the rigid confines of the eye socket (orbit). The exophthalmos of Grave’s ophthalmopathy represents spontaneous forward orbital decompression.
The eyelids, orbital tissues, and optic nerve limit this process. They connect the eye to the brain. The muscles that move and hold the eye also set boundaries.
Graves’ ophthalmopathy links with thyroid problems. We view both as autoimmune disorders.
The body’s host inflammatory cells, for some reason, attack specific tissues around the eye. These target tissues are usually the orbital fat, the directional eye muscles, and the muscles in the eyelid.
When tissues become inflamed in a specific manner, a distinct change occurs. This change creates the typical look of thyroid eye disease. This disease involves the eyelid muscles. Consequently, the eyelids retract, broadening the eyes’ opening. More white shows above and below the cornea. This condition results in a “stare” or bulging eye appearance. Interestingly, this happens even without the presence of exophthalmos. Moreover, orbital fat congestion plays a role too.
Indeed, it adds to actual exophthalmos. It also emphasizes fat pads in the upper and lower eyelids. Therefore, eyes appear puffy and shadow lines form.
Graves’s Disease and bloodshot eyes
Sometimes there is redness in the thin conjunctiva overlying the white portion of the eye, which gives the appearance of bloodshot eyes. When the eye muscles are inflamed, they may underact causing the eyes to move to different degrees, resulting in double vision (diplopia). In a small percent of patients, there is a significant inflammation of the eye muscles and orbital fat and in the very back portion of the orbit (apex), which may decrease the blood flow to the optic nerve.
 This can lead to subtle or profound loss of vision over either a short period of time or over a more progressive time course. The patient may subjectively experience diminished visual clarity, decreased color vision, or shadows or holes in the field of vision. Vision loss can affect one side, known as unilateral.
This can lead to subtle or profound loss of vision over either a short period of time or over a more progressive time course. The patient may subjectively experience diminished visual clarity, decreased color vision, or shadows or holes in the field of vision. Vision loss can affect one side, known as unilateral.
This condition can impact both sides, hence termed bilateral. Frequently, it remains undetected. A person may only realize it when closing one eye. Then, they examine each eye’s vision separately.
Most symptomatic patients present with mild ocular symptoms. These are similar to dry eye complaints. Some may feel a dull pressure or pain behind the eye. Yet, they don’t show all the listed abnormalities. These are just the clinical findings.
Medical Treatment
Early and mild eye symptoms include dryness, redness, itching, swelling of the eyelids, and the inability to wear contact lenses.
You can often treat these symptoms with frequent lubricating eye drops. Avoid over-the-counter eye whiteners. They can worsen the condition over time.
Wraparound sunglasses can relieve glare. Some patients find bedtime use of lubricating eye ointment beneficial. A bedside humidifier can help keep the room air moist. This can reduce dry eye symptoms.
Be cautious in environments with air conditioning and hot air heating. Windy days can also be troublesome. These conditions can exacerbate dry eyes.
A few patients will develop double vision. While awaiting either spontaneous improvement or surgical correction, some patients do well with prism lenses in their spectacles.
You can find temporary plastic press-on prisms. They’re cheaper and attach to glasses. You can replace them when needed.
Prednisone is a steroid medication you take orally. It offers short-term pain, swelling, and redness relief. Symptoms frequently come back after discontinuing the medication. Its side effects could limit the duration of use. However, severe cases are rare. Vision loss from pressure on the optic nerve happens to less than 5% of Graves’ disease patients.This is grave, indeed. A combination of treatments may be necessary. Prednisone, radiotherapy, and surgery could be used either separately or together to restore vision.
Despite these challenges, there’s a silver lining. It’s important to remember that slow, steady improvement is typical in Graves’ eye disease.
Surgical Management
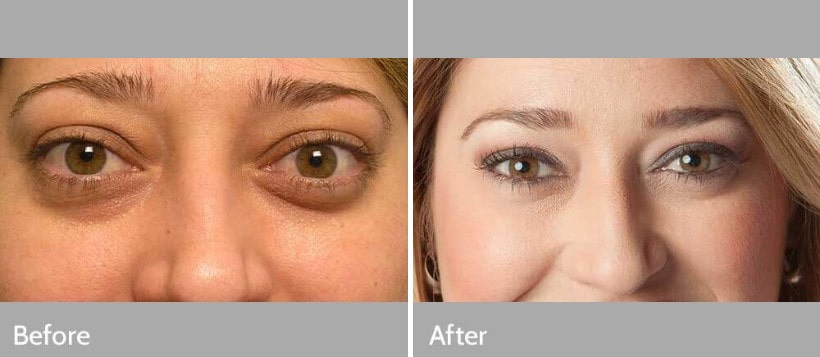
The retracted and puffy eyelids that have not improved with either medical management or time can alter a person’s appearance and self-esteem and increase the risk of drying of the cornea. Corrective eyelid surgery consists of adjustable loosening of the eyelid retractor muscles and release of scar tissue to bring the eyelids into a more normal position.
Excessive fatty tissue and skin folds may harm appearance. Surgeons can trim these to enhance looks. The surgery is outpatient-based. Most patients accept it readily.
Double vision or diplopia is a key issue for some patients. It comes from uneven scarring and eye muscle inflammation. If it persists without self-correction or prism glasses, surgery is necessary.
This surgery consists of detaching and repositioning the eye movement muscles on the eyeball to improve ocular alignment and minimize the double vision.
 Inflammation and Scarring
Inflammation and Scarring
The buildup of inflammation and scarring behind the eye may sometimes cause significant forward protrusion of the eye, which increases the disfigurement and ocular exposure. In 5% of Graves disease patients, the swelling in the orbit may actually contribute to progressive visual loss due to pressure on the optic nerve.
Orbital decompression surgery widens the eye socket. This is to make room for extra tissue behind the eye. It lets this tissue expand into nearby sinus cavities. Then, the eye can return to a more normal position.
Doctors suggest orbital decompression for patients with bulging eyes. It’s also recommended for those with vision loss or severe cornea exposure. Sometimes, doctors remove fat from behind the eye. This can happen alongside or instead of bone decompression.
They typically perform the surgery under general anesthesia. Most patients stay overnight in the hospital.
There is usually a significant improvement in the first week, which continues slowly over the next several months in 90% of the patients. The main risks of this procedure are double vision, numbness of the cheek and lip, and possible visual loss. Graves’ disease patients should be followed by an ophthalmologist experienced with the above conditions and treatments.
New Update August 2022: New data from Phase 2 and Phase 3 clinical trials demonstrated that the drug teprotumumab-trbw significantly improves symptoms of thyroid eye disease (TED) in different patient subgroups, with most maintaining a long-term response.