Hashimoto’s Hypothyroidism is one of the most increasingly common autoimmune disorders. It comes in various forms but they’re all characterized by abnormally low levels of thyroid hormones T4 and T3. There are also various causes but the most common cause globally is still iodine deficiency simply because a huge number of people with the condition live in countries where health policies addressing iodine deficiency do not exist.

In most developed countries, initiatives such as iodized salt and the addition of iodine to certain staple food products like dairy and even bread have resolved iodine deficiencies. In these countries, Hashimoto’s disease has become the single most common cause of hypothyroidism.
It is is also known as Hashimoto’s thyroiditis or Hashimoto’s disease. It gets its name from Dr. Hakaru Hashimoto, the Japanese doctor who first described this thyroid gland disorder that would eventually bear his name.
Hashimoto Disease – An Autoimmune Disorder
Hashimoto’s thyroiditis is classed as autoimmune thyroiditis. In an autoimmune disease your immune system begins to attack your body’s own cells.
There is a very complex cellular process by which this happens that is beyond the scope of this article.
Hashimoto’s Thyroiditis
Essentially though when you develop Hashimoto’s disease, your immune system attacks your thyroid gland and the resulting inflammation in the thyroid causes it to reduce, or stop, producing thyroid hormones.
The precise trigger that causes your immune system to develop thyroid self-antibodies (antibodies that attack the body’s own tissue) remains unknown. A bacterium or a virus might cause it, or it could primarily stem from genetic factors.
As thyroid hormone production declines due to Hashimoto’s disease, the thyroid receives signals from the pituitary gland to make more. This cycle may result in a goiter.
Who Commonly Gets Hashimoto’s Thyroiditis?
 Whilst all age groups and both males and females can get it, Hashimoto’s Thyroiditis, also known as chronic lymphocytic thyroiditis, most commonly occurs in middle aged women. If you also have a family history of thyroid disease your chances of developing it increase too.
Whilst all age groups and both males and females can get it, Hashimoto’s Thyroiditis, also known as chronic lymphocytic thyroiditis, most commonly occurs in middle aged women. If you also have a family history of thyroid disease your chances of developing it increase too.
Apart from this, people who have other autoimmune diseases have higher risk factors of developing Hashimoto’s disease, particularly those with rheumatoid arthritis, lupus or type 1 diabetes.
Excessive amounts of radiation exposure have also been associated with increased cases of Hashimoto Thyroiditis. However, if you suffer from Hashimoto’s disease or other types of autoimmune thyroid disorders, harmful side effects may result from your sensitivity to too much iodine.
How is Hashimoto’s disease diagnosed?
-
First, your healthcare provider will check your medical history and perform a physical examination followed by some blood tests.
-
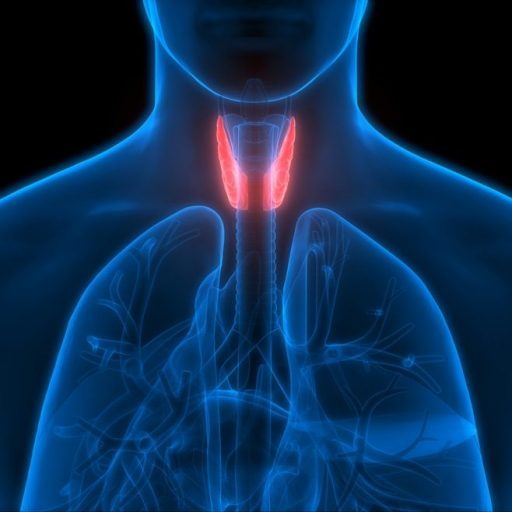
They will feel your thyroid gland to determine if it is enlarged. The thyroid is a small, butterfly-shaped gland in the front of your neck.
-
A blood test tells whether you have the antibodies that suggest Hashimoto’s disease. More than one in 10 people have the antibodies but have normal thyroid function. Having only the antibodies does not cause hypothyroidism.
-
TSH Test: The pituitary gland releases TSH (Thyroid Stimulating Hormone) when the system does not have enough thyroid hormone present.
Find out if you develop symptoms of Hashimoto’s Hypothyroidism?
 As is the case with most symptoms of thyroid disease, they’re slow to develop and often mistaken for other disorders with similar symptoms. Because postmenopausal women often exhibit its predominance, people can easily mistake many of the symptoms for that condition and overlook them accordingly.
As is the case with most symptoms of thyroid disease, they’re slow to develop and often mistaken for other disorders with similar symptoms. Because postmenopausal women often exhibit its predominance, people can easily mistake many of the symptoms for that condition and overlook them accordingly.
Sometimes someone with Hashimoto’s thyroiditis may develop goiter, which is when the thyroid swells. As the disease progresses, symptoms worsen and it’s at this point that many people begin to realize they could have thyroid problems.
The symptoms of Hashimoto’s disease are typical of hypothyroidism and include:
- Depression
- Constipation
- Tiredness
- Sluggishness
- Intolerance for cold
- Dry, pale skin
- Weight gain
- Puffiness around the eyelids and nose
- Alopecia (hair loss)
- Swollen tongue
- Brittle nails
- Sore stiff muscles and muscle weakness
- Pain and stiffness in joints
- Menorrhagia or, less commonly, amenorrhea
- The front of your neck may appear enlarged.
- Memory fog and lapses
Other factors that result in the need for continual monitoring of thyroid function (incl. thyroid hormone levels):
- previous thyroid surgery
- radioactive iodine treatment
- radiation therapy to the upper torso
- anti-thyroid medications
Hashimoto’s Hypothyroidism: Potential Complications of the Thyroid Gland
Over time, the ability of the thyroid gland to produce thyroid hormones often becomes impaired and leads to a gradual decline in function and eventually an underactive thyroid (Hypothyroidism). As is the case with all types of hypothyroidism, left untreated it will not only lead to a worsening of symptoms but will also cause severe health problems as the disease progresses.

- Goiter – under the pressure of continuous stimulation to produce thyroid hormones, your thyroid gland might eventually swell. An Enlarged thyroid may make swallowing and breathing difficult
- Heart disease, an enlarged heart and potentially heart failure – thyroid hormones help regulate blood levels of low-density lipoprotein cholesterol (LDLs). A drop in these thyroid hormone levels is often linked to a rise in LDLs
- Increasing depression
- Mental health issues causing a decline in well-being
- Sluggish mental functions and memory loss
- Decreased libido
- Myxedema and potentially myxedema coma, which is often fatal.
We also know that babies born to women who do not receive treatment for hypothyroidism face a higher risk of experiencing birth defects, along with brain, heart, and kidney disorders. These children also often end up with developmental and intellectual problems.
How is Hashimoto’s disease treated?
When Hashimoto’s disease progresses to hypothyroidism, doctors typically treat it with a synthetic form of thyroid hormone called levothyroxine (Synthroid®, Tirosint®, Levoxyl®, Levothroid®, Unithroid®). This drug restores the normal function of the thyroid.