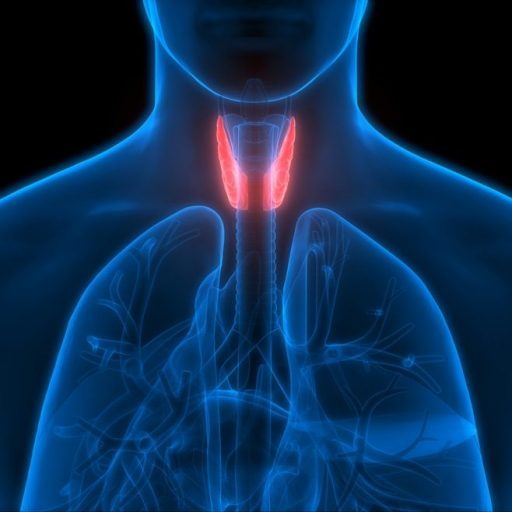
In my personal journey, I’ve come to understand that there are 7 distinct types of goiters, each associated with an enlarged thyroid gland. From what I’ve observed and learned, women seem to be more frequently affected. Sharing my insights, I’ve noticed that goiters can manifest in various forms like toxic, nontoxic, diffuse, and nodular, to name a few. Each type has unique characteristics and effects on thyroid hormone production, which can lead to different symptoms and health outcomes.
Toxic multinodular goiter
According to Penn Medicine, toxic multinodular goiter primarily affects older women, especially those over the age of 60 or who are post-menopausal. In my personal journey with this condition, I came to understand that it’s characterized by several autonomously functioning thyroid nodules (AFTNs) that produce thyroid hormones independently. The overproduction of these hormones leads to a state of hyperthyroidism. Symptoms commonly associated with this condition can range from heat intolerance, increased sweating, unintentional weight loss, to psychological symptoms such as anxiety and irritability.
Importantly, not all nodules within the same goiter are toxic. Non-toxic nodules do not secrete hormones, and therefore, their presence doesn’t contribute to the hyperthyroid state. The diagnosis of this condition is typically confirmed through tests such as fine needle aspiration biopsy, ultrasound, or a radioactive iodine uptake test. Treatment options often involve radioactive iodine therapy, anti-thyroid medications, or surgical removal of the gland.
Nontoxic multinodular goiter
Women with this condition have multiple thyroid nodules, but none of them affect the production of thyroid hormones. Because these nodules do not influence hormone levels, women often remain asymptomatic, although the goiter’s size may cause local symptoms like hoarseness, difficulty swallowing, or even a visible neck mass. Ultrasounds, physical examination, and fine needle aspiration biopsies are standard diagnostic methods for this type of goiter. Regular monitoring of the size and nature of these nodules is crucial even if they don’t affect hormone levels. Large goiters that cause symptoms or cosmetic concerns can be treated with surgery.
Toxic nodular goiter or toxic adenoma
This condition involves a single autonomously functioning thyroid nodule (AFTN) that produces an excess of thyroid hormones, leading to hyperthyroidism. The overactive nodule is often palpable and can cause symptoms including rapid or irregular heartbeats, nervousness, weight loss, and irregular menstrual periods in women. Diagnostic tests like thyroid function tests, ultrasound, and thyroid scans are used to identify and monitor the overactive nodule. Treatment often includes anti-thyroid drugs, radioactive iodine therapy, or even surgery in severe cases.
Diffuse toxic goiter
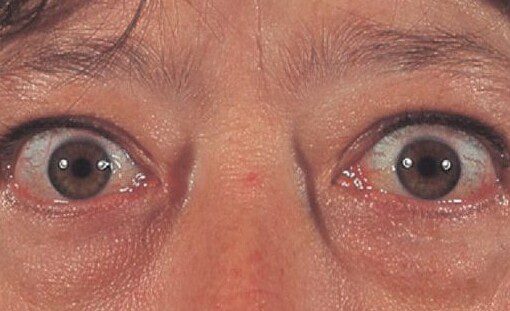
During my interactions with my endocrinologist and referring to the Cleveland Clinic, I learned that diffuse toxic goiter, commonly identified as Graves’ disease, results in the entire thyroid gland enlarging and overproducing thyroid hormones. From my observations and verified medical sources, many women with this condition report significant symptoms consistent with hyperthyroidism. Those symptoms include increased heart rate, hand tremors, unexplained weight loss, and changes in the menstrual cycle. Graves’ disease can also lead to eye problems like bulging eyes or double vision. Treatment options include anti-thyroid medications, beta-blockers to manage symptoms, radioactive iodine to reduce hormone production, or surgery to remove the thyroid.
Nontoxic goiter
Whether nodular or diffuse, this condition refers to an enlarged thyroid gland that does not affect hormone production levels. Despite the enlargement, hormone levels in the body remain normal. Women with this condition, also called sporadic goiter, may notice a lump in their neck, but they do not experience hormonal symptoms. However, the enlarged gland may cause physical discomfort, difficulty swallowing, or a noticeable mass in the neck. Regular monitoring is essential to ensure that the goiter doesn’t grow or become toxic. If the goiter continues to grow or symptoms become bothersome, surgery may be recommended.
Endemic goiter
From both my own research and discussions with healthcare professionals, especially the insights from the National Library of Medicine, it’s evident that endemic goiter frequently emerges in regions where diets are deficient in iodine, impacting a considerable segment of the community. One widely recommended approach, which I also found beneficial, is iodine supplementation to optimize thyroid functionality.
Retrosternal or substernal goiter
In my journey, one of the intriguing discoveries was about retrosternal or substernal goiter. Based on the guidance I received from my healthcare provider and corroborated by the Clayman Thyroid Center, this condition typically originates as a multinodular goiter extending into the upper chest region. For a comprehensive understanding, diagnostic measures frequently entail imaging studies to ascertain the goiter’s size and spread.
This downward growth may lead to pressure symptoms in the chest like shortness of breath, difficulty swallowing, or a feeling of pressure in the neck or chest. Despite the goiter’s unusual location, it may not affect hormone production, and women with this type of goiter may not experience typical symptoms of thyroid dysfunction. Diagnosis often involves imaging studies, such as chest X-rays, CT scans, or MRIs, to evaluate the size and extent of the goiter. The primary treatment is surgical removal to alleviate symptoms and prevent further complications.
Different Types of Goiter – Different Symptoms – Different Solutions
Each of the above conditions pertains to different types of goiter, a health concern often experienced by women, particularly those over 60 or post-menopausal. The types range from toxic multinodular goiter, with several hormone-producing nodules, to nontoxic goiter, which does not affect hormone production, to the substernal goiter that extends into the chest. These conditions can present unique symptoms, from hormonal imbalances to physical discomfort, requiring different treatment and management approaches.
Living with Goiter
Upon my diagnosis, supported by insights from Per Cramon, I discerned that the emotional challenges of living with a goiter can mirror its physical manifestations. The conspicuous changes in my neck combined with its daily implications were sometimes overwhelming for me. Here are some recommendations:
- Acknowledge your feelings: As someone who has lived with this condition, I’ve weathered days of intense anxiety, fear, and frustration. However, referencing psychological insights from the British Thyroid Foundation, I realized that allowing oneself the room to vent these emotions can significantly impact the coping process.
- Educate yourself: Knowledge is power. Understanding your specific type of goiter, its effects, and management plans can help you feel more in control. You’re less likely to fear the unknown when you know what’s happening.
- Communicate with your healthcare provider: Don’t hesitate to voice any concerns or ask questions about your condition or its treatment. They can provide answers, reassurance, or even adjustments to your treatment plan.
- Reach out for support: Lean on friends, family, or support groups. It can be comforting to share experiences and hear from others who’ve walked a similar path.
- Prioritize self-care: From both my experience and studies I’ve read from Arhanta Yoga, it’s beneficial to engage in activities that foster relaxation and well-being, such as yoga or meditation. Furthermore, consistent physical activity is often cited to assist in symptom management and mood elevation.
- Consult a mental health professional: There were moments when the emotional weight seemed too much for me to bear alone. Reaching out and consulting with a psychologist was a turning point. Their coping strategies were invaluable, and I’d recommend anyone going through similar challenges to consider this step.
Remember, you’re not alone in this journey. By acknowledging your feelings, arming yourself with knowledge, seeking support, and taking care of your overall health, you can better manage the emotional toll of dealing with these types of goiters.